Selective Laser Trabeculoplasty (SLT) is an advanced medical procedure primarily used to treat open-angle glaucoma, a condition characterized by increased intraocular pressure (IOP) due to impaired drainage of aqueous humor. SLT leverages the principles of selective photothermolysis to enhance the outflow of fluid from the eye, thereby reducing IOP. Unlike traditional laser surgeries that employ continuous laser beams, SLT uses short pulses of low-energy light, making it a gentler option with fewer side effects.
History and Development
The journey of laser surgery in ophthalmology began in the 1960s with the successful application of laser technology to treat retinal conditions. The development and refinement of laser techniques continued over the decades, leading to innovations in various ophthalmic surgeries. In the late 1990s, Dr. Mark Latina and colleagues introduced SLT as a distinct non-thermal laser therapy, focusing on the specific treatment of open-angle glaucoma.
SLT gained FDA approval in 2001 and has since become a widely accepted and effective alternative to traditional glaucoma treatments like medications and invasive surgeries. Its safety, efficacy, and minimal recovery time have contributed to its growing popularity within the ophthalmic community.
Applications and Uses
The primary application of SLT is in the management of open-angle glaucoma, where it assists in lowering IOP by improving aqueous humor outflow through the trabecular meshwork. This treatment is particularly beneficial for patients who:
Do not achieve sufficient IOP reduction with medications.
Experience significant side effects from glaucoma medications.
Seek to reduce their dependence on long-term glaucoma medications.
Ongoing research is exploring the potential of SLT in treating other forms of glaucoma, such as angle-closure and secondary glaucomas, along with conditions like anterior segment inflammation and uveitis. The non-invasive nature of SLT makes it an attractive option for a broader range of ophthalmic conditions.
Mechanism of SLT Laser Surgery
How SLT Laser Works
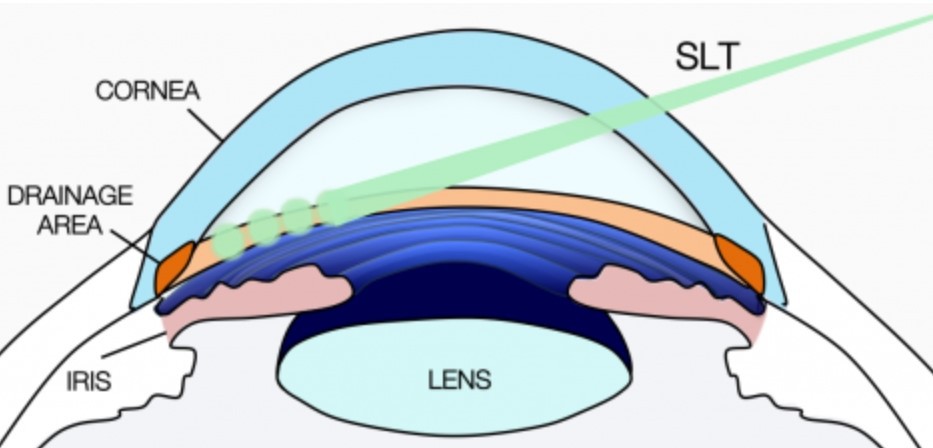
SLT laser surgery operates on the principle of selective photothermolysis, a process where laser energy targets specific pigmented cells while sparing the surrounding non-pigmented tissues. The SLT laser emits short pulses of green laser light at a wavelength of 532nm, which is selectively absorbed by the pigmented trabecular meshwork cells containing melanin.
These pigmented cells absorb the laser energy, leading to a series of biological responses that enhance the outflow of aqueous humor through the trabecular meshwork. These responses include:
Cellular activation: The absorbed energy stimulates resident macrophages and other cells to clear out debris and other blockages in the trabecular meshwork.
Remodeling of extracellular matrix: The laser-induced stimulation leads to structural changes in the trabecular meshwork that facilitate better fluid drainage.
Target Tissues and Cells
SLT specifically targets the trabecular meshwork, a spongy tissue located around the base of the cornea responsible for draining aqueous humor from the eye. The trabecular meshwork consists of pigmented endothelial cells that contain melanin, which selectively absorbs the laser light during SLT.
By focusing the laser energy on these pigmented cells, SLT induces minimal thermal damage to the non-pigmented cells and surrounding tissues, preserving the overall integrity of the trabecular meshwork and minimizing the risk of adverse effects.
Comparison to Other Laser Surgeries
SLT distinguishes itself from other laser surgeries such as Argon Laser Trabeculoplasty (ALT) through its selective, non-damaging approach. ALT uses continuous wave argon laser light, which can cause thermal damage and scarring to the trabecular meshwork. SLT, on the other hand, minimizes such risks with its low-energy, short-pulse laser, providing a safer and equally effective option.

Preoperative Preparations
Patient Counseling and Education
Effective patient counseling and education are critical components of preoperative preparations for SLT laser surgery. Patients should be thoroughly informed about:
The purpose and benefits of the procedure.
The expected outcomes and potential risks.
The steps involved in the surgery and postoperative care.
Providing patients with comprehensive information helps to set realistic expectations and ensures they are well-prepared for the procedure.
Medical History and Examinations
A thorough review of the patient's medical history and a comprehensive ocular examination are essential for determining their suitability for SLT. Key aspects of the preoperative assessment include:
Detailed ocular history: Gathering information on previous eye conditions, surgeries, and treatments.
Measurement of IOP: Assessing the current intraocular pressure to establish a baseline.
Gonioscopy: Examining the anterior chamber angle to confirm the diagnosis of open-angle glaucoma.
Visual field testing: Evaluating the extent of any vision impairment due to glaucoma.
Optic Nerve and Retinal Examination: A thorough examination of the optic nerve head and retina using techniques such as optical coherence tomography (OCT) and fundus photography helps assess the extent of glaucoma damage and rule out other ocular conditions that might influence treatment outcomes. This examination ensures that the patient is an appropriate candidate for SLT and allows for better monitoring of therapeutic success.
Informed Consent
Obtaining informed consent is a critical aspect of preoperative preparation. The patient should be provided with detailed information about the procedure, potential risks, benefits, and alternatives. This conversation typically covers:
Explanation of the SLT technique and its mechanisms.
Discussion of potential complications and side effects.
Overview of postoperative care and follow-up requirements.
Assurance of confidentiality and the right to withdraw consent.
Patients should be encouraged to ask questions, and their understanding of the procedure should be confirmed before proceeding.
The SLT Laser Surgery Procedure
Detailed Step-by-Step Process
Preparation:
Patients are positioned comfortably in front of the slit lamp.
Topical anesthetic drops are applied to numb the eye.
A gonioscopic lens is placed on the cornea to provide a clear view of the trabecular meshwork.
Laser Application:
The SLT laser is calibrated, and the ophthalmologist adjusts the parameters based on the patient's specific needs.
Laser energy is applied to the trabecular meshwork in approximately 50 to 100 evenly spaced spots, using short pulses.
The entire procedure typically takes 5-10 minutes per eye.
Completion:
The gonioscopic lens is removed.
Anti-inflammatory eye drops may be administered to minimize postoperative inflammation.
Anesthesia Options
SLT laser surgery generally requires only topical anesthesia, which numbs the surface of the eye and ensures patient comfort without the need for injections or systemic medications. This approach minimizes risks and reduces recovery time.
Duration and Recovery Time
The SLT procedure itself is relatively quick, typically taking about 5 to 10 minutes per eye. Recovery time is minimal, with most patients experiencing only mild discomfort or redness that resolves within a few hours to a day. Patients can usually resume normal activities almost immediately, although they might be advised to avoid strenuous activities for a short period.
Postoperative Care and Protective Measures
Immediate Care After Surgery
Following the SLT procedure, the patient should receive immediate postoperative care, including:
Monitoring IOP: The patient's IOP is checked shortly after the procedure to ensure no immediate complications, such as an acute rise in pressure.
Anti-inflammatory medications: Patients may be prescribed anti-inflammatory drops for several days to reduce postoperative inflammation and discomfort.
Medications and Follow-Up Appointments
Patients should adhere to the prescribed medication regimen and attend all scheduled follow-up appointments. These appointments are crucial for:
Monitoring IOP: Regular check-ups help determine the effectiveness of the SLT procedure in reducing IOP.
Assessing eye health: Ongoing examinations ensure early detection and management of any complications, such as increased IOP or inflammation.
Adjusting treatment: The ophthalmologist may adjust medications or recommend additional treatments based on the patient's response to SLT.
Protective Measures for Long-Term Eye Care
To maximize the benefits of SLT and protect long-term eye health, patients should follow several protective measures:
Adherence to follow-up schedules: Consistent follow-up is essential for monitoring eye health and managing glaucoma.
Medication compliance: Patients should continue taking prescribed glaucoma medications unless advised otherwise by their ophthalmologist.
Eye protection: Wearing sunglasses with UV protection helps shield the eyes from harmful radiation.
Healthy lifestyle: Maintaining a healthy lifestyle, including regular exercise, a balanced diet, and avoiding smoking, can contribute to overall ocular health.
Awareness of symptoms: Patients should be aware of any changes in vision or eye discomfort and report these to their ophthalmologist promptly.
Risks and Complications
Common Risks Associated with SLT Laser Surgery
While SLT is generally safe and well-tolerated, like any medical procedure, it carries some risks. Common risks include:
Mild eye discomfort: Some patients may experience temporary discomfort, redness, or irritation following the procedure.
Increased IOP: Although rare, some patients may experience a mild and transient increase in IOP immediately after SLT.
Inflammation: Postoperative inflammation can occur, but it is typically mild and managed with anti-inflammatory drops.
Complications and Their Management
Though uncommon, more serious complications may arise, necessitating prompt medical attention:
Persistent increases in IOP: Rarely, SLT may lead to a sustained rise in IOP, requiring additional treatment or surgery.
Corneal edema: Swelling of the cornea may occur, leading to blurry vision. This is usually temporary and resolves with appropriate treatment.
Hyphema: Bleeding into the anterior chamber can occur but is usually self-resolving. Close monitoring and, if necessary, additional medical intervention can manage this complication.
Ocular inflammation: In rare cases, significant inflammation may arise, requiring extended use of anti-inflammatory medications or other interventions.
Failure to achieve desired IOP reduction: Some patients may not experience the anticipated decrease in IOP following SLT, and alternative treatments or repeat SLT may be recommended.
Long-Term Implications
Over the long term, the effectiveness of SLT can diminish, often necessitating repeat treatments. However, repeated SLT procedures generally maintain their safety and efficacy, allowing for continued management of IOP with minimal invasive intervention.
Recent Advancements and Future of SLT Laser Surgery
Technological Innovations
Recent advancements in SLT technology focus on improving precision, reducing energy requirements, and enhancing patient comfort. Some of these innovations include:
Automated laser delivery systems: These systems provide consistent and accurate laser application, minimizing variation and enhancing outcomes.
Enhanced imaging techniques: Advanced imaging modalities, such as three-dimensional optical coherence tomography (3D-OCT), offer detailed views of the trabecular meshwork, allowing for more precise targeting during SLT.
Low-energy SLT: Newer models of SLT lasers use even lower energy levels, further reducing the risk of complications while maintaining efficacy in lowering IOP.
Research and Ongoing Studies
Research on SLT continues to expand its applications and refine its techniques. Key areas of ongoing study include:
SLT for angle-closure glaucoma: Investigating the potential benefits and effectiveness of SLT in managing different types of glaucoma beyond primary open-angle glaucoma.
Combination therapies: Exploring the synergistic effects of SLT in conjunction with other glaucoma treatments, such as medication or micro-invasive glaucoma surgeries (MIGS).
Long-term outcomes: Monitoring the durability of SLT's IOP-lowering effects over extended periods to better understand the timelines for re-treatment and optimal management strategies.
Potential Applications Beyond Current Uses
The versatility of SLT technology opens up potential applications in treating various ocular conditions beyond glaucoma. Future research may explore:
Inflammatory eye conditions: Utilizing SLT's precise targeting to manage specific inflammatory conditions affecting the anterior segment of the eye.
Ocular surface diseases: Investigating the potential for SLT to modulate cellular responses in diseases of the ocular surface.
Neovascular glaucoma: Exploring the use of SLT in cases of neovascular glaucoma where abnormal blood vessel growth impacts IOP.
Conclusion
Selective Laser Trabeculoplasty (SLT) represents a significant advancement in the management of glaucoma, offering a safe, effective, and minimally invasive treatment option for reducing intraocular pressure. Its precise targeting of the trabecular meshwork cells ensures a reduced risk of complications, making it an increasingly preferred choice for patients and ophthalmologists alike.
The preoperative process, including thorough patient counseling, medical assessments, and obtaining informed consent, is crucial in ensuring optimal outcomes. The SLT procedure itself is swift and usually well-tolerated, with minimal recovery time. Postoperative care, including medications and follow-up appointments, is essential for monitoring success and managing any potential complications.
While SLT is generally safe, like any medical procedure, it carries some risks and potential complications, which can be effectively managed with appropriate medical intervention.
The future of SLT is promising, with ongoing research and technological innovations poised to expand its applications and enhance its efficacy. As advancements continue, SLT may find broader uses in treating various ocular conditions, further solidifying its role in modern ophthalmic practice.
Patients considering SLT should engage in open discussions with their ophthalmologists to understand the full scope of the procedure, its benefits, risks, and long-term implications. By doing so, they can make informed decisions and take proactive measures to protect their vision health effectively.
In summary, SLT laser surgery is a transformative approach to glaucoma management, combining safety, efficacy, and precision. With ongoing research and a commitment to patient-centered care, SLT continues to pave the way for improved outcomes and better quality of life for those affected by glaucoma and potentially other ocular conditions in the future.